

Missing teeth change more than your smile: they alter how you bite, how your face supports surrounding tissues, and how easily you enjoy everyday foods. Modern implant dentistry rebuilds the entire tooth—root and crown—so you regain reliable chewing function, protect jawbone health, and enjoy an appearance that blends with the rest of your teeth. For many people, implants offer a long-term path back to normal eating and confident conversation.
At mediDental care we emphasize predictable biology and careful planning. Our approach focuses on minimally invasive placement, accurate restorative fit, and practical maintenance strategies so your implant solution performs well for years. Below you’ll find clear explanations of how implants work, what treatment typically involves, and how to choose clinicians and technologies that support dependable outcomes.
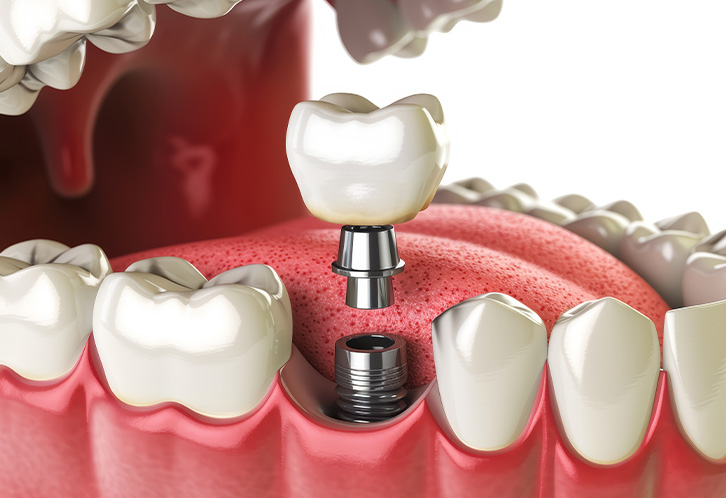
A modern dental implant is a small, biocompatible post—typically titanium or a titanium alloy—placed into the jawbone where a natural tooth root once was. That post becomes the structural anchor for the visible tooth replacement. Because it occupies the root space, the implant transfers chewing forces into the bone in a way that mimics a natural tooth, which is essential for long-term stability.
The key scientific principle behind implant durability is osseointegration: new bone grows tightly against the implant surface, creating a stable, living connection. Successful integration depends on good surgical technique, healthy bone volume, and appropriate timing between placement and restoration. Careful preoperative imaging and planning greatly increase the likelihood of predictable bone response.
After integration, a small connector called an abutment joins the implant to the final restoration—a crown, bridge, or denture. Separating function into implant (for biology), abutment (for fit), and restoration (for appearance and chewing) allows each component to be optimized. The result is a replacement that functions and looks like a natural tooth while remaining serviceable and maintainable over time.
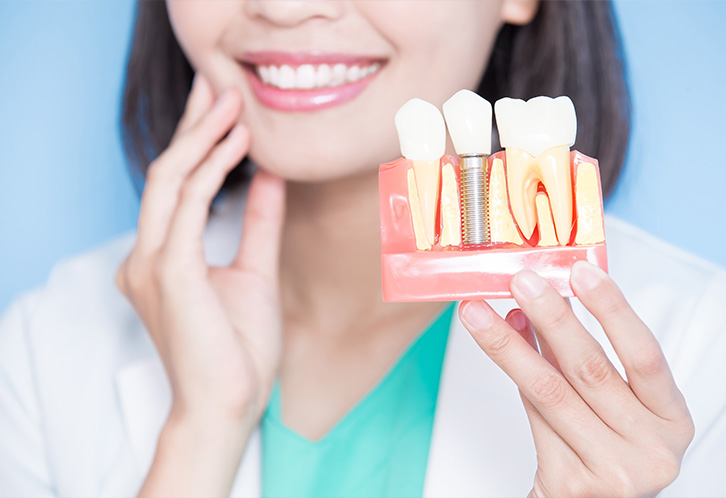
One of the most important differences between implants and removable dentures or traditional bridges is their effect on bone. Because implants transmit functional forces to the jaw, they help preserve bone volume and the contours of the face that can otherwise shrink after tooth loss. Maintaining that support reduces the sunken appearance that sometimes develops after multiple teeth are lost.
Implants also let clinicians avoid altering adjacent healthy teeth in many cases. A conventional bridge often requires reshaping neighboring teeth to support the restoration; implants can replace a single tooth without compromising surrounding tooth structure. For patients who value a conservative, long-term solution, that preservation of natural teeth is a significant advantage.
With appropriate home care and routine professional checks, implants are a dependable option for single-tooth replacement, partial gaps, and full-arch rehabilitation. Their success rests on matching sound surgical placement with prosthetic precision and consistent maintenance to catch any early changes in tissue health or mechanical stability.
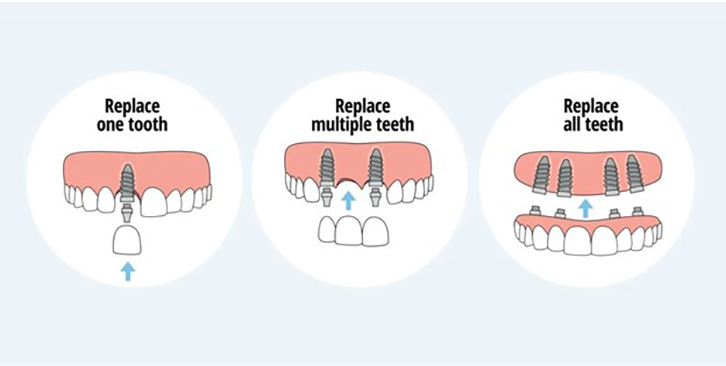
Treatment plans are customized to the number of missing teeth, the quality and quantity of jawbone, and each person’s functional and aesthetic goals. A single missing tooth is often restored with one implant and a custom crown. Multiple missing teeth can be addressed with several implants supporting individual crowns or a fixed bridge, which restores chewing power and improves oral hygiene accessibility.
For people missing many or all teeth, implant-supported full-arch options provide stable, long-term results. Solutions range from implant-retained overdentures to fixed, screw-retained prostheses using strategic configurations such as All-on-4® or All-on-6. These designs reduce the need for removable appliances while delivering predictable function and improved comfort.
Some patients require preparatory procedures—bone grafting or soft-tissue augmentation—to create the conditions needed for predictable implant placement. Thoughtful staging, clear timelines, and open communication about whether immediate restoration or a staged approach is best help patients make informed choices and achieve durable outcomes.

The process starts with a focused evaluation: a clinical exam, detailed medical and dental history, and digital imaging—often cone-beam CT—to visualize bone anatomy. Digital planning helps map critical structures, anticipate prosthetic needs, and design guides that improve placement accuracy. This preparation reduces surprises and helps set realistic expectations for timing and results.
Surgery is typically performed under local anesthesia with sedation options available for additional comfort. Implant placement is a controlled procedure with most patients experiencing only brief postoperative discomfort. A healing interval follows to allow osseointegration; temporary restorations can often be used so function and appearance are maintained during this phase.
Once integration is confirmed, the restorative phase begins. Abutments and final restorations are crafted to match your bite, speech, and smile. Digital impressions and CAD/CAM fabrication contribute to precise fit and natural aesthetics. After delivery, routine follow-ups monitor tissue health and prosthetic fit to keep the restoration functioning smoothly for years.
Successful implant outcomes combine surgical skill, restorative expertise, and coordinated follow-up care. When evaluating a provider, look for clinicians who either have implant training and restorative experience or who collaborate closely with specialists so both placement and reconstruction are planned together. That coordination reduces surprises and improves functional results.
At the practice level, consistent clinical protocols for infection control, treatment sequencing, and postoperative care contribute to predictable outcomes. mediDental care emphasizes clear communication so patients understand each step—from diagnostics to final restoration—and know how to support implant health with daily hygiene and timely professional visits.
Common issues, such as soft-tissue inflammation around an implant or mechanical wear of a restoration, are manageable when caught early. Regular maintenance appointments and good home care substantially reduce risk and help protect both the appearance and function of an implant restoration over the long term.
Advances in three-dimensional imaging, computer-guided planning, and digital impression techniques have raised the predictability of implant therapy. Cone-beam CT scans reveal bone volume and vital anatomy, while guided-surgery workflows translate the digital plan into precise implant positioning in the mouth. These tools reduce chair time and help align surgical results with prosthetic goals.
Digital impressions and CAD/CAM restorations support accurate fit and consistent occlusion, which are important for long-term mechanical stability. High-quality restorative materials and screw-retained designs make repairs and maintenance more straightforward when adjustments are needed. Together, modern tools and materials help clinicians deliver results that match patient expectations for function and appearance.
Ultimately, technology is most effective when combined with clinical judgment. A skilled team uses these tools to assess candidacy, manage risk, and create an individualized plan that reflects each patient’s anatomy and lifestyle.
Long-term implant health depends on a combination of good home care and professional oversight. Daily cleaning to remove plaque at the gumline, attention to the condition of surrounding soft tissues, and periodic assessments of bone levels at maintenance visits all help detect early changes. Preventive care is the most reliable way to protect function and aesthetics over time.
Be alert for signs that warrant prompt attention: persistent redness or swelling near an implant, unusual pain, changes in how a restoration fits, or noticeable changes in bite. Early evaluation often allows simple, effective interventions—improving the chances of preserving the implant and surrounding tissues.
When issues arise, collaborative care between surgical and restorative clinicians helps determine whether nonsurgical management, minor adjustments, or more involved procedures are needed. With timely action and consistent maintenance, many implants remain healthy and functional for decades.
Dental implants provide a biologically sound, long-lasting option for replacing missing teeth while preserving jawbone and restoring normal chewing function. Whether you need a single crown, several implants to fill gaps, or a full-arch restoration, careful planning and coordinated care make predictable outcomes possible for many patients. Candidacy depends on bone and gum health, general medical factors, and a personalized treatment plan that reflects individual goals.
If you would like to learn more about implant options in Bayside, NY, or to discuss whether implants are the right choice for you, please contact us for more information. Our team is available to explain the process and help you evaluate the best path forward.
If you've lost a tooth due to injury, decay, gum disease, or any other reason, we recommend dental implants to replace missing teeth. Dental implants come the closest to replicating the look, feel, and function of your natural teeth.
Dental implants are placed into the jawbone and mirror the same function as the root of a tooth. The procedure for dental implants is usually performed while a patient is sedated. Patients who undergo IV sedation must have an empty stomach and transportation home following the procedure. Most sedation patients will have little to no memory of the procedure occurring.
Generally, dental implants are made out of a biocompatible metal such as titanium. Biocompatible metals are also used for other common bone implants (such as shoulder, hip, and knee replacements). The visible portion of the implant is usually made out of porcelain and is custom-made to match your existing teeth.
Dental implants are designed to fuse to the bone, which makes them become permanent fixtures. Typically speaking, the success rate is nearly 100%. There are few cases in which the implant will not fuse as intended and must be removed. If this happens to occur, the procedure can be attempted again a few months later.
Dental implants are not usually covered by dental insurance, but may be covered under a patient's medical insurance. Our office and your insurance company can discuss coverage options with you based on your individual case and treatment plan.
It's easy... just take care of an implant as if it's a natural tooth! This involves regular brushing, flossing, and dental checkups. If you have any concerns about your implant, contact us immediately.