
Losing a tooth alters more than your smile: it changes how you chew, how your face is supported, and how neighboring teeth respond over time. Implant restorations recreate the complete tooth structure — an anchored root, a connecting abutment, and a custom prosthetic — to restore both appearance and everyday function. When planned with care, these restorations become a long‑term solution that patients often describe as feeling like their original teeth.
Because implant restorations are designed to integrate with the jaw and support the bite, they address problems that removable replacements cannot. Restorations anchored to implants help maintain bone volume, prevent unwanted tooth movement, and provide stable chewing without relying on adjacent teeth for support. The result is a more natural bite, improved speech, and a confident smile that’s easier to maintain over the years.
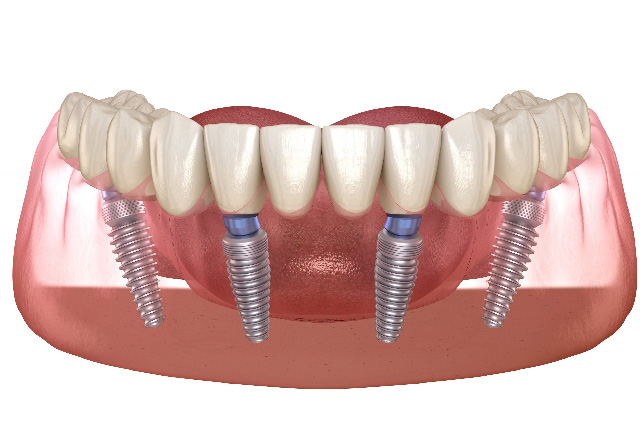
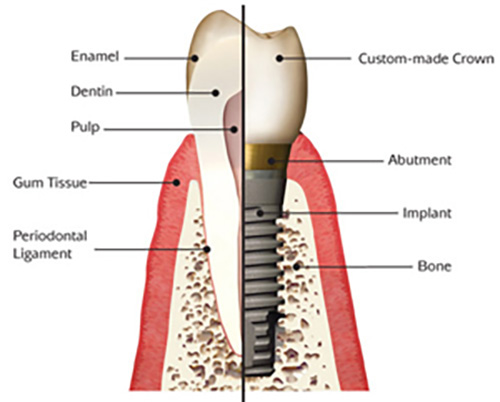
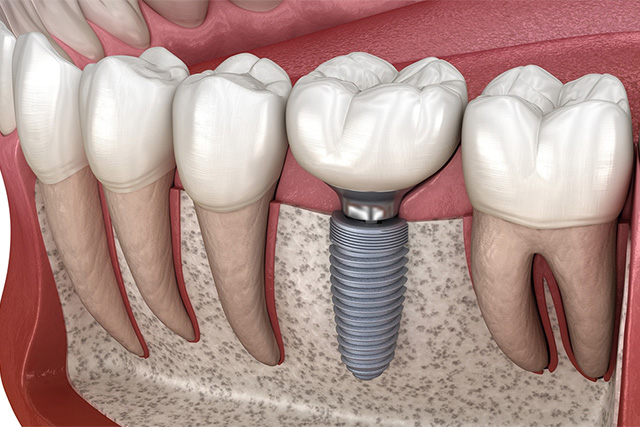
Unlike partial dentures or traditional bridges, implant restorations replace the missing tooth root as well as the visible crown. A biocompatible implant becomes an anchored foundation in the jawbone, an abutment connects the implant to the prosthetic, and a precisely shaped crown or bridge completes the tooth. This three‑component approach restores biting forces in a predictable way and keeps the prosthesis firmly in place during daily activities.
That root‑level support matters for more than stability. By transmitting normal functional loads into the bone, implants help preserve the jaw’s shape and reduce the bone loss that follows tooth removal. Preserving this underlying structure helps maintain facial contours and prevents the gradual shifting of neighboring teeth that can complicate future care.
Implant restorations are highly adaptable. A single implant can support an individual crown, multiple implants can anchor a bridge without altering adjacent healthy teeth, and implant‑retained overdentures can transform the fit and reliability of complete dentures. Every design is chosen to match a patient’s bite, tissue contours, and aesthetic goals so the final result feels and looks balanced with the rest of the smile.
Reliable implant results start with thorough diagnostics. Digital X‑rays and 3D scanning reveal bone volume, the location of nerves and sinuses, and how teeth come together during function. These images let the team design implant positions that are prosthetically driven — in other words, placed where the final tooth restoration will perform best for both strength and appearance.
Computerized planning often leads to guided surgical techniques that translate the preoperative plan into precise placement at the time of surgery. This predictability reduces intraoperative surprises and supports smoother healing. When bone is insufficient for ideal placement, modern grafting and sinus lift procedures can rebuild the foundation so implants sit in the optimal position long term.
After an appropriate healing interval, detailed impressions or digital scans record the implant’s orientation and soft‑tissue form so the laboratory can fabricate crowns, bridges, or denture frameworks that match adjacent teeth in shade, shape, and occlusion. Chairside adjustments fine‑tune bite and comfort, ensuring the final restoration feels integrated with the patient’s natural dentition.
Implant restorations are suitable for many adults missing one or more teeth, but candidacy depends on a range of clinical factors rather than age alone. Essential considerations include the health of the gums, the amount and quality of jawbone available, and a patient’s ability to follow oral hygiene and recall visits. Patients with certain medical conditions can still be candidates after appropriate medical review and coordination with their physician.
Tobacco use, uncontrolled gum disease, and some systemic issues can affect healing and the long‑term prognosis of an implant. When such concerns are present, the clinical team will outline steps to optimize oral health prior to implant placement — for example, addressing periodontal inflammation or rebuilding bone so the implant rests on a stable foundation.
Every plan is individualized: options, expected timelines, and maintenance requirements are discussed clearly so patients understand the tradeoffs between restorative approaches. This collaborative planning helps people choose a treatment path that aligns with their functional needs, aesthetic priorities, and daily routines.
Following implant placement, short‑term symptoms such as swelling, mild discomfort, and tenderness are common and typically resolve with routine postoperative care. A soft diet, careful local hygiene, and adherence to scheduled follow‑ups support predictable tissue healing and successful integration of the implant with the jawbone. Early checkups allow the team to confirm progress and address any questions promptly.
Long‑term success depends on consistent home care and periodic professional assessments. While implants themselves are not susceptible to decay, the soft tissues around them can develop inflammation if plaque accumulates. Daily brushing, flossing or interdental cleaning around the abutment, and routine professional cleanings help prevent peri‑implant disease and detect wear or fit issues before they become problematic.
Prosthetic parts may require occasional maintenance — for example, adjustments to occlusion or replacement of worn components — but with attentive care an implant restoration can remain a stable, durable solution for many years. Prompt attention to changes in comfort, looseness, or function increases the likelihood of preserving the investment of time and treatment.
Excellent implant outcomes depend on a coordinated approach: clinicians who understand both surgical and restorative aspects, accurate diagnostics, and skilled laboratory technicians who craft the final prosthesis. Transparent communication among the team and with the patient keeps expectations aligned and reduces uncertainty at each stage of care.
Attention to patient comfort — through effective anesthesia, sedation options when appropriate, and a well‑paced treatment schedule — helps people navigate the process with minimal stress. Restorative choices are made with durability and hygiene in mind so the finished restoration is both long‑lasting and maintainable with realistic daily routines. At mediDental care, clinicians emphasize evidence‑based techniques and individual attention to achieve predictable, natural‑looking results.
If you’d like to learn whether implant restorations are the right option for your smile, the clinical team can review your history, examine your oral condition, and outline a personalized plan. Contact mediDental care for more information and to schedule a consultation.
In summary, implant restorations offer a stable, tooth‑supported way to replace missing teeth while preserving oral structure and function. If you’re considering this option and want to explore next steps, please contact us for more information — we’ll be happy to discuss how implant restorations might restore comfort, function, and confidence to your smile.